The following post is written by Andrew Blecher MD – you can follow him @the_jockdoc
Platelet Rich Plasma (PRP) therapy is a relatively new treatment designed to aid in the healing and regeneration of soft tissues such as tendons and ligaments. To fully understand the benefits of PRP therapy it is first useful to have some understanding of the basic science behind tendon and ligament injuries. Tendons and ligaments are made up of fibers of collagen. When these fibers are stretched or torn we may refer to the injury as a “pull”, “tear”, “sprain” (ligament) or “strain” (tendon). These structures are vascular which means there are blood vessels in them. Thus, when they are injured they bleed. If there is enough bleeding we may notice bruising around the area of injury. Blood flow to the area increases to aid in healing. The blood carries platelets and growth factors that allow for healing of the tissue by creating new collagen fibers. These new fibers need to be constructed in an organized, layered fashion to heal correctly and allow the ligament or tendon to regain its proper strength and flexibility.
Sometimes, however, the healing process does not work correctly and instead of forming healthy collagen fibers there is significant scar tissue that develops in its place. One of the risk factors for this is not getting enough blood flow to the area to provide those platelets and healing factors. The development of scar tissue even further inhibits proper blood flow as new capillaries and other small blood vessels can’t penetrate through the scar tissue to provide blood flow to the injured area. The new development of small blood vessels is called “angiogenesis” or “neovascularization”. When scarred or disorganized tissue inhibits this process the blood flow to the area becomes “blocked”. This means that the tissue will never really have the opportunity to heal correctly. That is why sometimes ligament and tendon injuries heal and other times they do not.
When these injuries don’t heal, patients often become frustrated. Patients may try anti-inflammatories and other pain medications, topical creams and gels, braces, physical therapy, massage, acupuncture and cortisone injections but nothing seems to work. That’s because these therapies may try to treat pain and inflammation but they don’t treat the underlying problem of scar tissue, disordered fibers and poor angiogenesis (blood flow). The result is that many patients may give up and live with pain and disability or may end up with surgery. PRP therapy is the solution to this problem. In PRP treatment the patient’s own blood is taken with a simple blood draw. Using a special centrifuge machine this blood is spun down to separate out and concentrate the platelets and growth factors that are essential for tissue healing. This small amount of fluid with concentrated platelets and growth factors is called platelet rich plasma (PRP). Nothing else is added to the patient’s own blood products so there is no risk of allergy, reaction or rejection. PRP therapy is a purely natural process using the body’s own healing factors. The trick is getting them to the right place. The physician uses a diagnostic ultrasound machine to identify the area within the ligament or tendon that is injured. The newest ultrasound technology provides resolution to see every millimeter of the collagen fibers as well as scar tissue and blood flow to the area. The physician is then able to use a needle to inject the PRP directly into the injured area and even between tightly packed collagen fibers. The PRP can even be injected directly into very small tears that are sometimes not apparent on MRI. Once these platelets and growth factors are in the area of injury they then become activated. They also recruit other healing proteins and factors to the area so that healing and regeneration of the tissue can now begin.
This therapy has been used extensively in Europe for several years and is now becoming more popular in the U.S. as more people become aware of its potential benefits and as more research is being done. But the idea of getting blood to an injured area is not new. For years many people have tried needling tissue or even injecting an irritant into the tissue (prolotherapy) to attempt to increase blood flow to the injured area. Now with the development of PRP we can actually get the specific healing factors within the blood to the injured area. This not only allows for healing of injuries which may not otherwise heal, but it also speeds up recovery of injuries which may eventually heal over a longer period of time. Thus PRP therapy is a great option for two different patient populations. One is the patient with the chronic injury that never seems to go away. The other is the patient with an acute injury which might otherwise take 8-12 weeks to heal and is looking to do something to “speed up” the recovery process. That is why PRP has become so popular among athletes and there have been many media reports of elite athletes receiving PRP treatment for injuries that occur mid-season or even right before big events such as the Superbowl. But PRP treatment is not just for athletes.
PRP therapy can be used with great success for the following conditions:
- Acute and chronic tendon injuries (tendonitis, tendinosis, tendinopathy, tendon tears)
- Foot and ankle: Plantar fasciitis, Achilles tendonitis and partial tears
- Knee: Patellar tendonitis and tears, Quadriceps tendonitis and tears
- Thigh: Hamstring strains
- Elbow: Medial epicondylitis (golfer’s elbow) and Lateral epicondylitis (tennis elbow)
- Shoulder: Rotator cuff tendonitis and partial tears
- Acute and chronic ligament injuries (sprains)
- And many other conditions associated with scarred or non-healing tissue.
In the case of patellar tendinopathy, PRP is extremely useful with cure rates of 80-90% in my experience. Patellar tendinopathy is the chronic breakdown of the patellar tendon in the knee. Patellar tendinopathy is commonly misdiagnosed and mistakenly referred to as “patellar tendinitis” or “jumper’s knee”. In the case of patellar tendinopathy the tendon develops micro-tearing and even sometimes significant partial tearing with the eventual development of scarring and thickening of the tendon. This is commonly found in athletes as a result of repetitive running, jumping or running up and down hills or stairs. Typical symptoms include chronic pain in the anterior aspect of the knee that is brought on or made worse with exercise. Typical treatments include anti-inflammatories, creams, ice, rest, physical therapy and massage. When these therapies fail patients are often left without other options. PRP is the perfect solution for these patients.
What to expect during your PRP treatment
First your physician will evaluate your injury and use musculoskeletal diagnostic ultrasound to closely examine the injured area and determine if you would be a good candidate for PRP treatment.
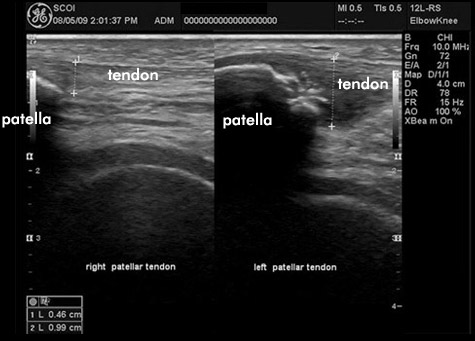
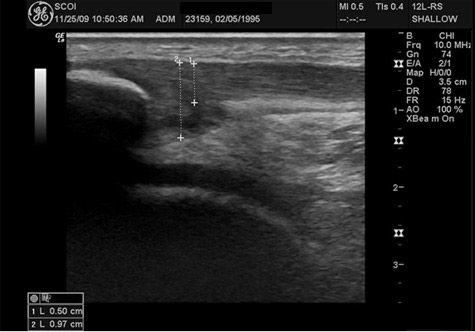
Below is an ultrasound comparison of a healthy patellar tendon (left) and patellar tendinopathy (right).
We recommend that you avoid taking anti-inflammatories (such as ibuprofen or naprosyn) or aspirin for at least one week prior to beginning PRP treatment. On the day of the treatment your blood will be drawn from a small vein in your arm. This blood will be placed into a special centrifuge machine designed specifically for producing platelet rich plasma. The separation and concentration process will take about 15 minutes to produce the platelet rich plasma.
Centrifuge
During this time your physician will re-evaluate the injured area with the ultrasound and pinpoint the exact area for treatment. The area will be anesthetized with a local anesthetic. The PRP is then drawn from the centrifuge into a syringe.
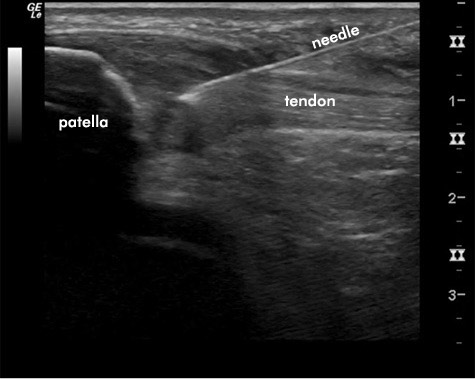
The concentrated platelet rich plasma will then be injected into the injured area using a long, thin needle under sterile procedure and ultrasound guidance.
The tendon is fenestrated and patellar spurring is debrided by the needle. Platelet rich plasma is then injected into the degenerated and thickened part of the patellar tendon. If a large partial tear is present then the PRP will be injected directly into the defect of the tear.
The entire office procedure should take approximately 40 minutes. Patients should expect mild discomfort but no pain during the procedure. In some cases, depending on the nature of the injury, a brace may be required to be worn for the first several days after the procedure. All soreness from the procedure should resolve within 48 hours and the patient should be able to resume all normal activities. Depending on the nature of the injury, physical therapy may be required during the healing process. If needed, a specialized rehabilitation program emphasizing eccentric strengthening will be personalized to your condition. The amount of time before all symptoms resolve and the tissue is fully healed will depend on the nature and extent of the injury and may range from 1-2 weeks to 1-2 months.
The patient will then be re-examined with musculoskeletal ultrasound to confirm tissue healing and that the problem is “cured.” Occasionally a second PRP treatment may be required if complete healing and regeneration has not occurred. However, in my experience, approximately 80% of patients experience significant if not complete resolution of symptoms after only one treatment.
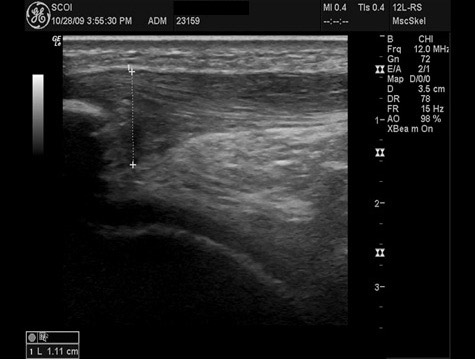
At one month after procedure, tendon is still thickened but most superior aspect now has good fiber alignment and organization. Patellar spurring diminished.
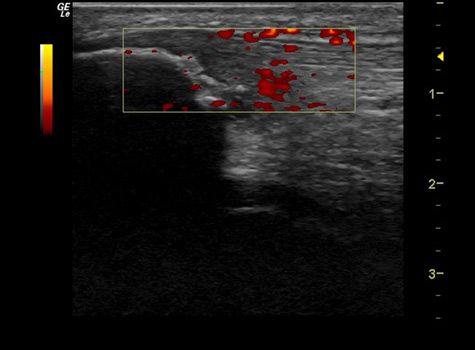
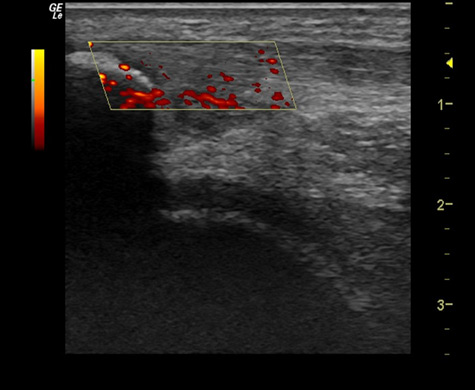
Doppler flow shows increased blood flow and healing response throughout tendon.
At 2 months post-procedure, now tendon has regenerated to normal thickness with excellent fiber organization. Patellar spurring has completely disappeared.
Blood flow through regenerated part of tendon has returned to normal.
PRP treatment certainly isn’t a miracle for everyone, but when used correctly it certainly can produce amazing results.
“Close to the end of the third game in our season, I was hit in the knee on a short yardage play and tore my MCL. It ended up being a grade 3 tear, and I was told the ligament would take 8-12 weeks to completely heal. I was the only person on the team that played center so it was important that I came back as soon as possible. The doctor suggested a PRP treatment. About a week after the injury I received a PRP treatment, and two weeks later I was back in practice. The doctor was amazed at how quickly my ligament healed. I hardly noticed any looseness or pain in my first game back. We’re in week ten of the season now and my knee doesn’t bother me at all!”
-Jackson Smith, College of the Canyons, Santa Clarita, CA
Website: BlecherMD
Follow me on twitter: @the_jockdoc